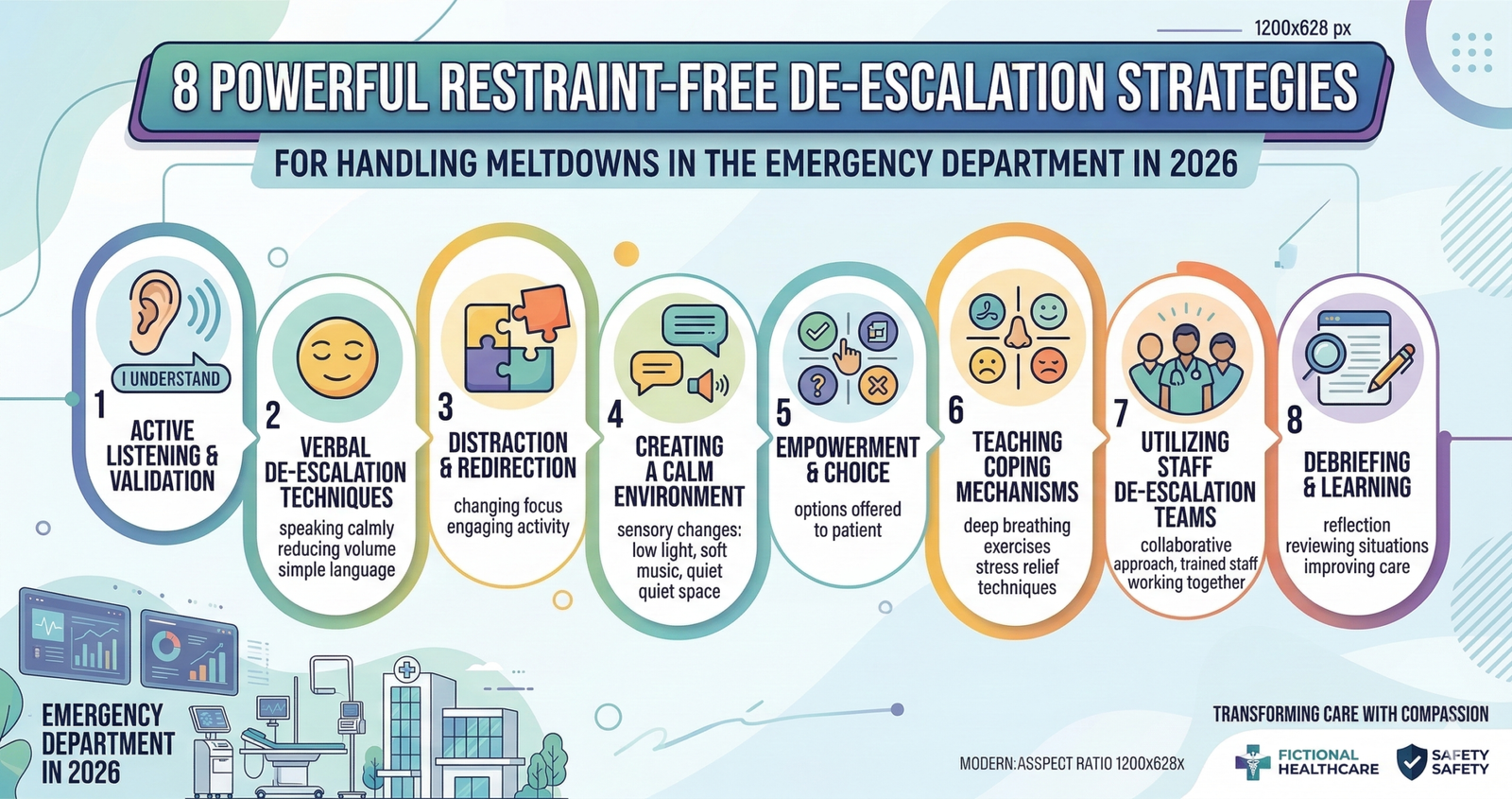
Explore 8 Powerful Restraint-Free De-escalation Strategies for Handling Meltdowns in the Emergency Department in 2026. 8 evidence-based restraint-free de-escalation strategies for managing meltdowns in the emergency department in 2026. Essential nursing guidance for neurodivergent-responsive acute care.
For Handling Meltdowns in the Emergency Department in 2026: 8 Powerful Restraint-Free De-escalation Strategies
To respond appropriately to patients experiencing emotional crises in emergency departments by 2026, a shift towards nonviolent, trauma-centered care is essential to reduce agitation and increase safety. Evidence-based de-escalation strategies emphasize co-regulation, where staff manage their own emotions to help patients regain control and thus reduce the need for physical restraints.
Introduction
When an autistic patient experiences a meltdown in the emergency department, the clinical response of the nursing team can either de-escalate the crisis or profoundly deepen it. A meltdown — a neurological response to sensory, emotional, or cognitive overload — is fundamentally different from a behavioral tantrum or psychiatric episode, yet it is frequently mismanaged through the lens of physical restraint and sedation in acute care settings.
The Autistic Self Advocacy Network (ASAN) reports that autistic individuals are disproportionately subjected to physical restraint during healthcare encounters, often resulting in physical injury, psychological trauma, and long-term healthcare avoidance. Research published in the Journal of Emergency Nursing confirms that restraint-free de-escalation techniques are not only safer for autistic patients but produce faster resolution of crisis episodes when applied by trained nursing staff. In 2024, restraint-free care is not aspirational — it is the evidence-based standard.
Understanding the Neuroscience of a Meltdown Versus a Behavioral Crisis
The single most important clinical distinction emergency nurses must make is between a meltdown — a neurologically driven loss of regulatory capacity — and a volitional behavioral crisis or psychiatric emergency. A meltdown occurs when the autistic nervous system reaches a threshold of sensory, emotional, or cognitive input that it can no longer process, triggering a dysregulated state that the individual cannot voluntarily control or stop.
Neuroscientist Stephen Porges’ Polyvagal Theory illuminates this process precisely — describing how the autonomic nervous system shifts from social engagement into fight-or-flight or dorsal vagal shutdown states under conditions of perceived threat or overwhelm. Unlike a behavioral outburst driven by intent, a meltdown represents a temporary collapse of neurological self-regulation. Treating it with physical restraint activates additional threat pathways, intensifying rather than resolving the crisis and risking significant physical and psychological harm to the patient.
Recognizing Early Warning Signs Before a Meltdown Escalates
Effective restraint-free de-escalation begins long before a meltdown reaches its peak — it begins at the first observable signs of nervous system dysregulation. Early warning indicators, sometimes called the “rumble stage,” include increased motor restlessness, repetitive self-stimulatory behavior, vocal changes such as humming or echoing, facial flushing, visible tension in the jaw or hands, reduced verbal responsiveness, and withdrawal from eye contact or social interaction. These signals constitute a clinical window of opportunity during which nursing intervention can prevent full meltdown escalation.
The Incredible 5-Point Scale, developed by Kari Dunn Buron and Mitzi Curtis, is a validated tool used by nurses and support teams to identify and communicate escalation levels in autistic individuals. Emergency nurses trained to read these early cues carry the most powerful de-escalation tool available — early, calm, and informed intervention before the neurological threshold is crossed.
The CALM Framework — A Nursing De-escalation Model for Neurodivergent Patients
Several structured de-escalation frameworks have been adapted specifically for neurodivergent patients in acute care settings. The CALM approach — Communicate clearly, Adjust the environment, Limit demands, and Monitor at a safe distance — provides emergency nurses with a memorable, stepwise protocol for responding to meltdowns without physical intervention. Clear communication means using short, simple, concrete sentences delivered in a calm, low-pitched tone, avoiding rhetorical questions, commands framed as choices, or rapid verbal exchanges that overwhelm auditory processing.
Environmental adjustment involves immediately reducing sensory input — dimming lights, silencing unnecessary alarms, clearing bystanders, and offering a quieter space. Limiting demands means temporarily withdrawing all clinical expectations and allowing the patient’s nervous system to begin its own recovery arc. Monitoring at a safe distance ensures patient safety without the intrusive physical proximity that prolongs dysregulation in autistic individuals.
Sensory De-escalation Tools Every Emergency Department Should Have Accessible
Equipping emergency department nursing teams with sensory de-escalation resources is a low-cost, high-impact structural investment that reduces meltdown duration and restraint rates significantly. Core sensory tools include noise-canceling headphones, weighted blankets, sunglasses or eye masks to reduce light sensitivity, handheld fidget devices, oral sensory tools for patients who seek proprioceptive input, and portable white noise machines. The Hospital Sensory Kit model, piloted and published by the Autism Speaks Healthcare Initiative, documents consistent reductions in patient distress and staff-reported escalation rates in departments where these kits were made accessible at triage.
Nurses should also be aware that for some autistic patients, deep pressure input — such as wrapping oneself tightly in a blanket — is a voluntary, self-regulatory behavior that should be facilitated rather than restricted. Distinguishing self-regulatory sensory behaviors from self-injurious behaviors requires clinical training, observational skill, and genuine knowledge of the individual patient.
Communication Strategies That Reduce Escalation During Meltdown Episodes
Language and communication approach are among the most powerful variables a nurse controls during a meltdown response. The foundational principle is reduction — fewer words, simpler sentences, longer pauses, and a quieter voice consistently outperform directive, explanatory, or reassurance-heavy communication styles during acute neurological dysregulation. Nurses should avoid saying “calm down,” “look at me,” or “tell me what’s wrong” phrases that impose demands on a nervous system that has temporarily lost its capacity to comply.
Instead, brief validating statements such as “You are safe,” “I am not going to hurt you,” and “You do not have to talk right now” delivered slowly and quietly help activate the ventral vagal social engagement system described in Porges’ Polyvagal Theory. For patients with AAC devices or communication boards, making these tools accessible and visible during the meltdown — without requiring their use — preserves the patient’s communication autonomy while reducing the pressure to perform verbally under acute distress.
The Role of Caregivers in Restraint-Free Meltdown Management
In emergency department settings, the autistic patient’s caregiver or family member is frequently the most effective de-escalation resource available to the nursing team. Caregivers possess irreplaceable knowledge of the individual’s sensory triggers, preferred comfort strategies, effective communication approaches, and recovery timeline. Emergency nursing protocols must formally integrate caregiver involvement into meltdown response — actively inviting caregivers into the patient’s space, deferring to their behavioral guidance, and avoiding interventions that the caregiver identifies as contraindicated for their specific patient.
Jean Watson’s Theory of Human Caring, foundational in nursing philosophy, recognizes the therapeutic relational field that encompasses patient, family, and nurse as the authentic site of healing. Displacing or excluding caregivers during a meltdown — a common reflexive response in busy emergency settings — removes the patient’s most trusted co-regulator and significantly prolongs crisis duration.
Legal, Ethical, and Human Rights Dimensions of Restraint Use in Autistic Patients
The use of physical restraint in autistic patients during meltdowns is not simply a clinical practice question — it is a human rights and legal accountability issue that nursing professionals cannot afford to approach casually. The United Nations Convention on the Rights of Persons with Disabilities (UNCRPD), ratified by over 180 nations, explicitly identifies freedom from non-consensual physical intervention as a fundamental right of disabled individuals in healthcare settings.
In the United States, The Joint Commission’s restraint and seclusion standards mandate that physical restraint be used only as a last resort when there is imminent risk of harm and no less restrictive alternative is available. The ANA Code of Ethics, Provision 1, requires nurses to practice with respect for the inherent dignity and rights of every patient, which directly implicates restraint decision-making in autistic populations. Nurses who document meltdown responses thoroughly — including all de-escalation attempts made prior to any restrictive intervention — protect both their patient and their professional practice.
Building an Emergency Department Culture of Neurodiversity-Affirming Restraint-Free Care
Sustainable, systemic change in how emergency departments respond to autistic patients in meltdown requires cultural transformation, not just individual clinical skill development. Nurse managers and clinical educators play a pivotal role in establishing neurodiversity-affirming care as a departmental value — embedding autism-specific de-escalation training into mandatory orientation and annual competency programs, designating Autism Champions within the nursing team, and creating clear escalation pathways that route autistic patients in crisis to trained staff and adapted environments rather than to restraint.
The Emergency Nurses Association (ENA) Position Statement on Care of the Autistic Patient explicitly calls for systemic changes in emergency nursing education, environmental design, and triage protocols to reduce preventable restraint use. Departments that track restraint rates in autistic patients as a formal quality indicator and review these cases in structured post-incident debriefs create the accountability infrastructure that drives lasting, measurable improvement in restraint-free care delivery.
Conclusion
Restraint-free de-escalation in the emergency department is both a clinical imperative and a moral obligation for the nursing profession in 2024. Autistic patients experiencing meltdowns are not behavioral problems to be managed — they are individuals in acute neurological distress who require informed, compassionate, and evidence-based nursing responses.
From recognizing early warning signs and applying the CALM framework to deploying sensory tools, integrating caregivers, and upholding human rights standards, every strategy in this post represents a concrete, achievable step toward safer and more equitable emergency care. For nursing students, emergency nurses, nurse educators, and clinical leaders, building competency in restraint-free de-escalation is not optional — it is the foundation upon which genuinely neurodiversity-affirming emergency nursing practice is built, one therapeutic encounter at a time.
FAQs
What is the key clinical difference between an autistic meltdown and a behavioral or psychiatric crisis?
A meltdown is a neurologically driven loss of self-regulation caused by sensory or cognitive overload — it is involuntary and cannot be stopped by the individual through will or compliance. A behavioral or psychiatric crisis involves different etiological pathways and requires distinct clinical assessment and intervention approaches.
What does the CALM de-escalation framework involve for autistic patients in the emergency department?
CALM stands for Communicate clearly, Adjust the environment, Limit demands, and Monitor at a safe distance. It provides emergency nurses with a structured, stepwise approach to meltdown response that reduces escalation without physical intervention or restraint.
When is physical restraint legally and ethically permissible for an autistic patient in meltdown?
Under The Joint Commission standards and the ANA Code of Ethics, physical restraint is permissible only as a genuine last resort when there is imminent risk of serious physical harm and all less-restrictive de-escalation alternatives have been attempted and documented as ineffective.
How can emergency nursing leaders build a sustained culture of restraint-free care for autistic patients?
Leaders can embed autism de-escalation training in mandatory nursing education, designate departmental Autism Champions, track restraint rates in autistic patients as a formal quality metric, and conduct structured post-incident debriefs to drive continuous, accountable improvement in neurodiversity-affirming care.
Read More:
https://nurseseducator.com/didactic-and-dialectic-teaching-rationale-for-team-based-learning/
https://nurseseducator.com/high-fidelity-simulation-use-in-nursing-education/
First NCLEX Exam Center In Pakistan From Lahore (Mall of Lahore) to the Global Nursing
Categories of Journals: W, X, Y and Z Category Journal In Nursing Education
AI in Healthcare Content Creation: A Double-Edged Sword and Scary
Social Links:
https://www.facebook.com/nurseseducator/
https://www.instagram.com/nurseseducator/
https://www.pinterest.com/NursesEducator/
https://www.linkedin.com/company/nurseseducator/
https://www.linkedin.com/in/afzalaldin/
https://www.researchgate.net/profile/Afza-Lal-Din
https://scholar.google.com/citations?hl=en&user=F0XY9vQAAAAJ