Learn Catatonia in Autism 2026: 10 Clinical Warning Signs of “Shutdown” Every Nurse Must Recognize. The ten important caution symptoms and symptoms of catatonia in autism in 2026. A nurse`s evidence-primarily based totally manual to spotting ASD shutdown, scientific evaluation tools, and remedy interventions.
10 Clinical Warning Signs of “Shutdown” Every Nurse Must Recognize: Catatonia in Autism 2026
Introduction
Catatonia is one of the maximum dangerous, maximum regularly missed, and maximum clinically complicated comorbidities related to Autism Spectrum Disorder (ASD). A 2022 meta-evaluation posted in npj Mental Health Research (Nature) protecting 969 people located that about 10.4% of human beings with ASD meet the standards for catatonia — with a few extra latest parental-file studies, consisting of Yürümez et al. (2024), figuring out incidence as excessive as 35.4% in youth elderly 12 to 18. Critically, Frontiers in Psychiatry (2024) reviews that catatonia consists of a 60-fold boom with inside the threat of untimely death, setting early identity through nurses firmly with inside the class of a life-saving scientific competency.
Despite this, catatonia in ASD stays chronically underdiagnosed, poorly understood, and mechanically harassed with behavioral regression or willful noncompliance. For nurses in developmental, psychiatric, inpatient, and number one care settings, expertise the way to understand the “shutdown” of autistic catatonia is an urgent, nonnegotiable scientific priority.
What Is Catatonia? Reframing a Misunderstood Diagnosis
Catatonia is a complicated neuropsychiatric syndrome characterized through a cluster of psychomotor disturbances related to motion, volition, speech, and behavior. Historically related to schizophrenia, catatonia is now identified through the DSM-five as an impartial specified relevant throughout diagnostic categories — consisting of as a proper modifier to ASD, a reputation that turned into itself a landmark development in neurodevelopmental psychiatric classification. The DSM-five defines catatonia through the presence of as a minimum 3 of twelve symptoms: catalepsy, waxy flexibility, stupor, mutism, negativism, agitation, posturing, stereotypy, mannerisms, grimacing, echolalia, and echopraxia.
For autistic people, however, the DSM-five standards on my own are broadly taken into consideration insufficient. A 2025 narrative assessment posted in PMC (PubMed Central), inspecting literature spanning 1943 to 2024, showed that sizeable symptom overlaps among catatonia and middle ASD functions — consisting of repetitive and confined behaviors, echolalia, posturing, and stereotypies — complicates the software of fashionable diagnostic standards.
Wing and Shah (2000), whose foundational paintings with inside the British Journal of Psychiatry stays the cornerstone of autistic catatonia research, proposed 4 defining diagnostic functions unique to the autistic catatonic presentation: markedly expanded slowness in motion and verbal responses, issue beginning and finishing actions, expanded reliance on activates from others, and expanded passivity with an obvious lack of motivation. Nurses should internalize this framework, because it displays what an autistic catatonic episode simply looks as if on the bedside — now no longer a dramatic frozen posture, however a quiet, modern withdrawal from practical engagement with the world.
The Neurobiological Basis: Why Autistic Brains Are Vulnerable to Catatonia
Understanding why autistic people are disproportionately at risk of catatonia calls for familiarity with the shared neurobiological mechanisms underlying each situation. The excitatory/inhibitory (E/I) imbalance that characterizes ASD — pushed through dysregulation throughout GABAergic, glutamatergic, serotonergic, and dopaminergic neurotransmitter systems — is now understood to be a number one contributor to catatonic vulnerability. A 2022 ultra-modern evaluate in npj Mental Health Research showed that neuroimmune disorder and genetic variations disrupting SHANK3 — scaffolding proteins important to synaptic structure — are a few of the maximum substantial diagnosed hazard elements for catatonia in neurodevelopmental populations.
Catatonia itself is increasingly theorized as an evolutionarily conserved freeze or shutdown reaction, at first defined through Moskowitz (2004) in Psychological Review as an intense fear-primarily based totally immobility reaction. In the context of ASD, an already beaten sensory and regulatory system — chronically working close to the brink of overwhelm — may also cause this neurological freeze reaction in reaction to stressors that might be conceivable for neurotypical people.
Medical situations consisting of autoimmune encephalitis, epilepsy, hormonal modifications at some point of puberty, and the unfavorable consequences of antipsychotic medicines have all been documented as precipitants or exacerbates of catatonia in autistic people. Nurses’ ought to recognize that catatonia in ASD isn’t always a behavioral choice — it’s far a neurological occasion with identifiable organic substrates and triggers.
10 Clinical Warning Signs of Autistic Catatonia Nurses Must Know
Autistic catatonia hardly ever provides as sudden, dramatic immobility. It is maximum normally a slow, insidious deterioration in characteristic that unfolds over weeks to months, making early nursing reputation significantly depending on an accurate, longitudinal expertise of the affected person`s baseline. The following ten caution signs, derived from Wing and Shah (2006), the Shah and Wing Assessment Blueprint, the Bush-Francis Catatonia Rating Scale (BFCRS), and medical steering from the Association for Science in Autism Treatment (ASAT), constitute the middle early and evolving signs nurses ought to study to identify.
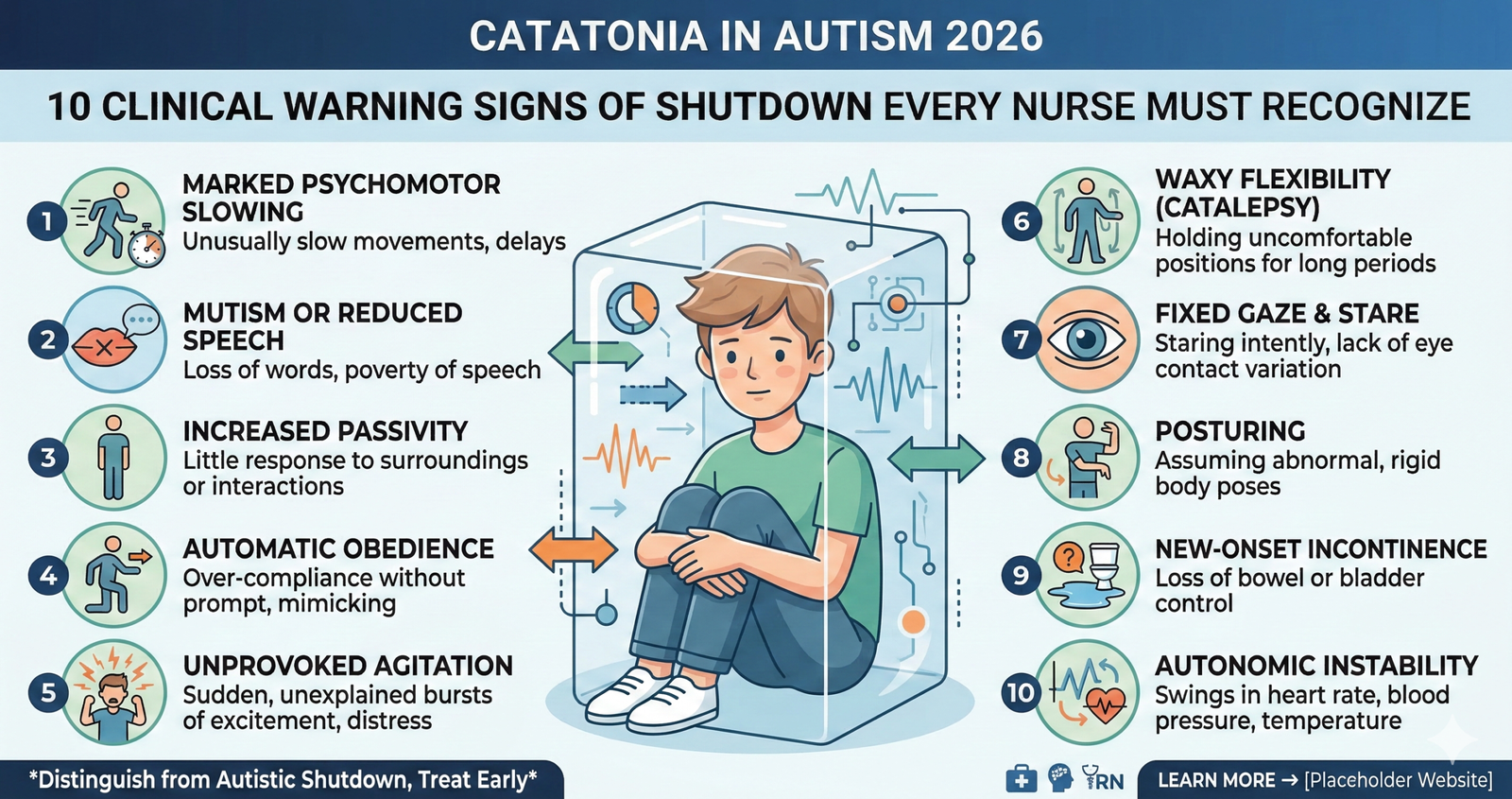
The first caution signal is markedly expanded slowness in motion and verbal responses — a affected person who formerly dressed independently now takes thirty mins to place on one shoe, or a affected person who communicated quite simply now speaks after a postpone of numerous seconds. The 2d is trouble beginning moves no matter obvious intent — attaining for an item and freezing mid-motion, or status in a doorway not able to pass the brink. The 0.33 is a dramatic growth in set off dependency, with the affected person requiring bodily or verbal cuing for duties formerly finished independently. The fourth is revolutionary social withdrawal and lack of formerly installed social engagement behaviors.
The 5th caution signal is surprising or modern lack of speech, consisting of discount in verbal output, mutism, or the emergence of echolalia and echopraxia. The 6th is new or markedly intensified repetitive moves and stereotypies that vary qualitatively from the affected person`s set up repertoire. The 7th is posturing — the affected person retaining unusual, anatomically awkward positions for extended intervals without obvious discomfort. The 8th is sizeable weight loss, dehydration, or deterioration in self-care bobbing up from issue starting up or finishing eating, drinking, and hygiene tasks.
The 9th is new onset of urinary or fecal incontinence in an affected person with set up toileting abilities, reflecting lack of volitional motor management in place of regression. The 10th — and significantly important — is catatonic excitement: paradoxical episodes of purposeless, disorganized motor interest or behavioral outbursts that seem without identifiable cause and aren’t in the individual’s managing. Nurses who stumble upon this 10th presentation are at the best chance of misinterpreting it as willful aggression or behavioral crisis, whilst it’s miles in truth a manifestation of catatonic neurological dysregulation.
Autistic “Shutdown” vs. Catatonia: A Clinical Distinction Nurses Must Make
The idea of autistic “shutdown” — a well-diagnosed shielding reaction wherein an autistic man or woman withdraws from sensory, social, and communicative engagement following overwhelm — stocks superficial similarities with catatonic presentation however is awesome in its mechanism, trajectory, and scientific management. Understanding this difference is vital for correct nursing evaluation and well-timed intervention.
Autistic shutdown is usually time-limited, resolving inside hours to days as soon as the overpowering stressor is eliminated and the man or woman has ok time in a safe, low-stimulation environment. It does now no longer contains the modern, week-length deterioration in formerly mastered abilities that characterize autistic catatonia. Catatonia, with the aid of using contrast, is persistent, escalating, and functionally disabling. It is no longer self-clear with relaxation or environmental amendment alone. A scholar with ASD who shuts down after a distressing college day and recovers after a quiet night at domestic is showing a strain reaction, now no longer catatonia.
A scholar with ASD who step by step loses the cappotential to provoke moves, stops eating, develops urinary incontinence, and calls for bodily prompting to walk — over the route of numerous weeks following a worrying lifestyles occasion — is providing with autistic catatonia and calls for pressing scientific evaluation.
Key precipitating stressors documented with inside the literature consist of grief and bereavement, college transitions, lack of routine, interpersonal conflict, reports of abuse or trauma, parental divorce, and the strain hole among highbrow cappotential and overall performance expectations — a sample mainly referred to in higher-functioning autistic younger human beings with the aid of using Wing and Shah (2000) and replicated in current publications. A 2024 ScienceDirect examine of three hundred individuals’ elderly 12 to twenty-five discovered that 25% of these recognized with catatonia had skilled a worrying lifestyles occasion with inside the previous six months, reinforcing the vital function of psychosocial records in nursing evaluation.
Clinical Assessment Tools: What Nurses Should Use
Formal medical evaluation of catatonia in ASD calls for verified gadgets which might be suitable for neurodevelopmental populations. The Bush-Francis Catatonia Screening Instrument (BFCSI) and its elevated version, the Bush-Francis Catatonia Rating Scale (BFCRS), are the maximum broadly used and clinically verified equipment for quantifying catatonia severity throughout inpatient and outpatient psychiatric settings. A 2024 Turkish validation look at posted in ScienceDirect diagnosed catatonia in 37.5% of forty-eight adolescent ASD sufferers the usage of the BFCRS — a locating that powerfully underscores the scale`s sensitivity whilst carried out with the aid of using educated clinicians.
The Attenuated Behavior Questionnaire (ABQ), advanced with the aid of using Breen and Hare (2017), changed into designed to seize the motor, effective, and behavioral dimensions of autistic catatonia that well-known catatonia scales might also additionally under detect. The ABQ validated terrific validity and reliability in a 2025 ScienceDirect look at (Spearman-Brown coefficient of 0.979), with a diagnostic cut-off of 92.5 and a screening cut-off of 39.5, making it the maximum ASD-unique evaluation alternative presently available.
The Shah and Wing (2006) “Blueprint for the Assessment of Catatonia in ASD” offers an extra complete framework requiring nurses to accumulate records from a couple of sources — parents, teachers, and former clinicians — and to assess extrade from the patient’s documented baseline throughout a couple of purposeful domain names along with motor movement, speech, self-care, eating, and toileting.
Nurses must additionally be aware of the lorazepam tasks look at, defined with the aid of using Dhossche (2014), which includes administering a take a look at dose of lorazepam and watching for a marked, if temporary, development in catatonic symptoms. A high-quality reaction to the lorazepam task offers sturdy diagnostic affirmation and courses the selection to provoke benzodiazepine remedy as a part of the formal remedy plan.
Treatment Approaches: From Lorazepam to ECT and Psychological Intervention
The remedy of catatonia in ASD is stratified via means of severity and is guided via way of means of a aggregate of pharmacological, mental, and environmental approaches. Benzodiazepines — maximum usually lorazepam — are universally diagnosed because the first-line pharmacological remedy for catatonia irrespective of the underlying etiology. The PMC “Decalogue of Catatonia in ASD” (Dhossche, 2014) states that benzodiazepines and bilateral electroconvulsive therapy (ECT) need to be taken into consideration secure and powerful clinical remedies for pediatric catatonia and catatonia in ASD, supported via means of case-document proof and scientific series.
Nurses should be conscious that ECT, even as commonly taken into consideration handiest for severe, life-threatening, benzodiazepine-refractory instances, has been mentioned in a couple of posted instances to provide sustained development in autistic catatonia without proof of cognitive or neuropsychological worsening, which includes in sufferers who’ve obtained preservation ECT for numerous years.
A similarly essential and proof-supported remedy pillar is the mental and environmental method recommended via means of Wing and Shah (2000) and encouraged via way of means of Autism Society (autism.org.uk). Their scientific version positions pressure and tension because the number one precipitants of catatonic breakdown in autistic people and recommends a mental method that identifies the specific, individualized stressor for every affected person and addresses it through complete mental evaluation and a holistic, multidisciplinary care plan related to the affected person, their caregivers, and neighborhood services.
This method without delay informs the nursing role: nurses are frequently the clinicians with the maximum sustained affected person contact, the maximum special longitudinal understanding of the affected person`s baseline, and the best ability to discover and speak the stressors that induced or hold the catatonic episode.
Critically, the Autism Society’s scientific steerage explicitly warns that a psychiatric medication — which includes antipsychotics — may also cause or get worse catatonia in autistic people. Nurses should report and speak about this hazard to the prescribing team, while autistic sufferers are admitted with behavioral displays which could set off a reflexive attain for antipsychotic agents. A drastic intervention, which includes high-dose lorazepam and ECT, needs to be reserved for severe, life-threatening catatonia that has did not reply to first-line approaches, in complete accordance with the scientific steerage issued via way of means of Dhossche, Shah, and Wing (2006) of their foundational International Review of Neurobiology framework.
The Nurse’s Role in Preventing Diagnostic Delay
One of the maximum consequential and habitual findings throughout the autistic catatonia literature is the profound diploma of diagnostic delay — frequently measured in years — that autistic sufferers enjoy earlier than catatonia is efficaciously diagnosed. A center motive for this delay, defined explicitly with inside the ASAT medical guidance, is that many healthcare experts are unaware that autistic catatonia exists, do now no longer understand its medical presentation with inside the autistic population, and can characteristic the affected person`s deterioration to behavioral regression, willful noncompliance, or worsening of the underlying ASD itself.
This misattribution effects with inside the utility of behaviorally targeted interventions — inclusive of extended behavioral needs, consequence-primarily based totally management, and at instances bodily restraint — that aren’t most effective useless however can be actively dangerous for a affected person in neurological shutdown.
Nurses are uniquely placed to interrupt this cycle of diagnostic delay. By retaining detailed, longitudinal documentation of an autistic affected person’s purposeful baseline; via way of means of spotting the early, diffused symptoms and symptoms of catatonic deterioration earlier than they attain disaster level; via way of means of advocating for formal catatonia evaluation the usage of confirmed gear; and via way of means of speaking medical worries truly and urgently to the multidisciplinary team, nurses can compress the diagnostic timeline that separates autistic sufferers from powerful remedy.
The distinction among catatonia diagnosed at its early, attenuated level and catatonia diagnosed in its severe, malignant form — characterized in Frontiers in Psychiatry (2024) as wearing dangers of pneumonia, deep vein thrombosis, strain ulcers, rhabdomyolysis, malnutrition, dehydration, and death — is the distinction that skilled, knowledgeable nursing evaluation can make.
Conclusion
Catatonia in autism is a serious, probably life-threatening, and chronically under recognized neuropsychiatric comorbidity that needs pressing interest from the nursing career in 2025. Affecting an anticipated 10% to 35% of autistic youth and adults relying on evaluation methodology, autistic catatonia affords now no longer as dramatic immobility however as an insidious “shutdown” a revolutionary withdrawal from movement, communication, and self-care this is without difficulty wrong for behavioral regression or willful noncompliance.
Nurses who recognize the Wing and Shah diagnostic framework, the 10 medical caution symptoms and symptoms, the confirmed evaluation gear inclusive of the BFCRS and ABQ, and the stratified remedy approach — from individualized mental intervention via to lorazepam and ECT — are ready to be the primary line of protection towards this risky and underdiagnosed condition. For nursing students, clinicians, educators, and researchers, learning catatonia in ASD isn’t always a sophisticated distinctiveness niche — it’s miles a center medical duty with inside the transport of safe, evidence-primarily based totally, and life-defensive take care of autistic sufferers throughout each care setting.
FAQs
How is autistic catatonia different from an autistic “shutdown”?
An autistic shutdown is a temporary, stress-brought on withdrawal that resolves inside hours to days as soon as the triggering stressor is removed. Autistic catatonia is a persistent, modern neurological syndrome concerning lack of formerly mastered motor, communicative, and self-care competencies over weeks to months, which calls for formal medical evaluation and established scientific or mental intervention to treat.
What evaluation equipment need to nurse use to display screen for catatonia in ASD?
The Bush-Francis Catatonia Rating Scale (BFCRS) is the maximum broadly established medical tool for catatonia severity throughout psychiatric settings. The Attenuated Behavior Questionnaire (ABQ) is the maximum ASD-unique tool, demonstrating awesome reliability in a 2025 validation study. Together with the Shah and Wing (2006) Assessment Blueprint, that equipment offer nurses with a comprehensive, evidence-primarily based totally screening framework.
What is the first-line remedy for catatonia in autistic patients?
Benzodiazepines — maximum typically lorazepam — are the first-line pharmacological remedy for catatonia in ASD, frequently showed diagnostically thru a lorazepam undertaking test. Alongside pharmacotherapy, a mental technique concentrated on the unique man or woman stressor that brought about the catatonic episode is strongly recommended, especially for slight to slight displays. ECT is reserved for severe, remedy-refractory, life-threatening cases.
Can antipsychotic medicines motive or get worse catatonia in autism?
Yes. Clinical steerage from Wing and Shah (2006), encouraged with the aid of using the National Autistic Society (autism.org.uk), explicitly warns that psychiatric medicines — together with antipsychotics — can cause or get worse catatonia in autistic individuals. Nurses need to record this threat actually and talk it to the prescribing team, especially while behavioral displays set off attention of antipsychotic agents.
Read More:
https://nurseseducator.com/didactic-and-dialectic-teaching-rationale-for-team-based-learning/
https://nurseseducator.com/high-fidelity-simulation-use-in-nursing-education/
First NCLEX Exam Center In Pakistan From Lahore (Mall of Lahore) to the Global Nursing
Categories of Journals: W, X, Y and Z Category Journal In Nursing Education
AI in Healthcare Content Creation: A Double-Edged Sword and Scary
Social Links:
https://www.facebook.com/nurseseducator/
https://www.instagram.com/nurseseducator/
https://www.pinterest.com/NursesEducator/
https://www.linkedin.com/company/nurseseducator/
https://www.linkedin.com/in/afzalaldin/
https://www.researchgate.net/profile/Afza-Lal-Din
https://scholar.google.com/citations?hl=en&user=F0XY9vQAAAAJ