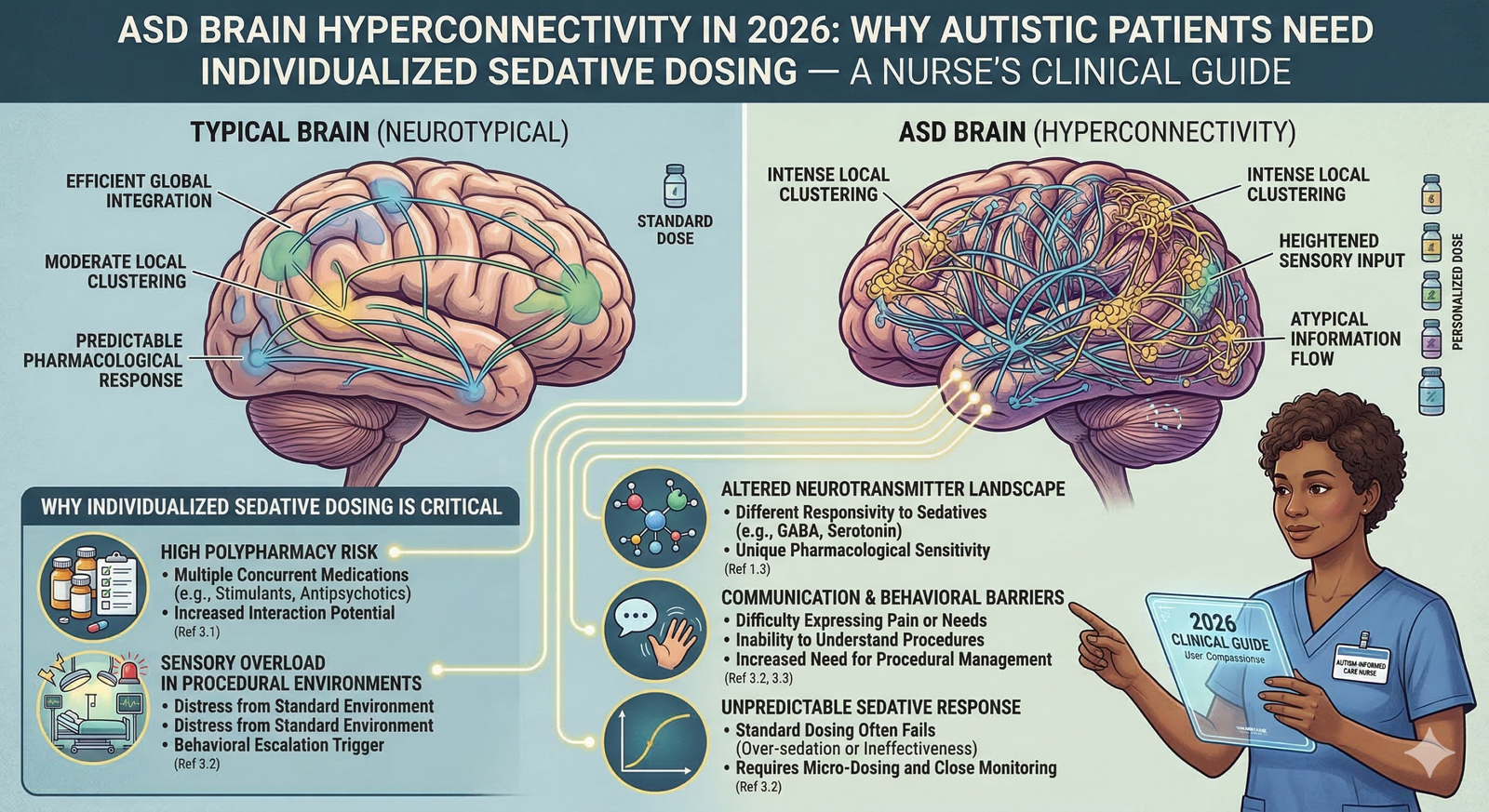
Discover ASD Brain Hyperconnectivity in 2026: Why Autistic Patients Need Individualized Sedative Dosing — A Nurse’s Clinical Guide. Why did ASD mind hyperconnectivity influence sedative dosing in 2026. A nurse`s evidence-primarily based totally manual to perioperative care, drug considerations & the Autistic SPACE framework.
Why Autistic Patients Need Individualized Sedative Dosing — A Nurse’s Clinical Guide: ASD Brain Hyperconnectivity in 2026
Introduction
Caring for autistic sufferers in perioperative and procedural settings is one of the maximum nuanced scientific demanding situations nurses face today. At least 1 to 2% of humans are autistic, and greater than 110,000 autistic kids go through surgical operation with inside the United States annually — with hundreds greater requiring sedation for diagnostic imaging, EEG recording, and dental procedures.
A foundational but regularly disregarded thing shaping sedation care on this populace is mind hyperconnectivity: a neurobiological phenomenon that basically alters how autistic brains reply to sedative and anesthetic dealers. For nurses, knowledge of this mechanism isn’t a non-obligatory specialty — it’s far a vital factor of security, evidence-primarily based totally perioperative exercise in 2025.
What Is Brain Hyperconnectivity in ASD? The Neuroscience Nurses Must Know
Brain hyperconnectivity in ASD refers to an ordinary sample of immoderate or deregulated purposeful connectivity throughout large-scale cortical and subcortical neural networks. In neurotypical people, the mind continues a cautiously regulated stability among neural excitation and inhibition — a dynamic recognized clinically because the excitation/inhibition (E/I) ratio. In ASD, this stability is disrupted, with excitatory signaling predominating and generating a country of world or nearby hyperconnectivity that persists even at rest.
A landmark Bio Rxiv evaluation primarily based totally on 657 autistic people recognized essential neurological subtypes in ASD: one characterized with the aid of using hypoconnectivity and one with the aid of using hyperconnectivity. Approximately 42% of autistic topics verified the hyperconnective subtype, with enriched expression of genes related to E/I imbalance — organizing a clean genomic and neurophysiological foundation for the distinction.
Separately, studies posted in PMC verified that mTOR-based elevated synaptic backbone density is at once related to cortico-striatal hyperconnectivity and autism-like behavior, and that kids with idiopathic ASD show a similar connectivity fingerprint to those animal models. These findings offer the molecular framework nurses want to apprehend why autistic brains do now no longer reply to sedative dealers the manner neurotypical brains do.
A 2025 Brain Sciences review (MDPI) similarly showed that sensory processing variations in ASD rise in large part from dysregulation of arousal circuits that is itself a downstream outcome of ordinary cortical connectivity. Nurses should internalize this connection: an autistic patient’s hyperconnected, hyperaroused mind calls for a basically distinct pharmacological and environmental method to reap secure and powerful sedation.
The Sedation Paradox: Why Dosing in ASD Is More Complex Than Standard Protocols Suggest
The medical photo of sedation necessities in ASD is nuanced and does now no longer suit smartly right into an unmarried directional claim. A 2024 potential observational look at posted in Acta Paediatrica as compared sedative necessities among youngsters with ASD and neuro-abnormal controls present process MRI below dexmedetomidine sedation. The findings found out that youngsters with ASD required better anesthetic doses to obtain immobility while imaging as compared to youngsters without ASD — a locating that demanding situations the belief that hyperconnectivity universally interprets to decreased sedative necessities.
At the equal time, a compelling frame of proof from the Autism Research Institute — authored via way of means of a licensed registered nurse anesthetist (CRNA) and figure of an autistic child — highlights that many anesthesia carriers reflexively over-sedate autistic sufferers in reaction to behavioral presentations, without effectively accounting for underlying metabolic vulnerabilities together with mitochondrial dysfunction, impaired methylation pathways, and abnormal hepatic metabolism.
This CRNA`s medical observations, drawn from extra than 25 years of practice, explicitly advise coming near autistic sufferers the manner one could method sufferers with hepatic or renal impairment: with a heightened stage of individualized pharmacological respect, the use of the fewest tablets essential on the maximum cautiously titrated doses to obtain the medical intention.
This obvious paradox — that a few autistic sufferers require better doses for procedural immobility whilst others can be extra prone to negative results from popular dosing — underscores the essential significance of individualized evaluation as opposed to protocol-pushed dosing. Nurses must apprehend that no unmarried sedation dosing method applies throughout the heterogeneous autistic population, and that the medical intention is usually individualized, now no longer standardized.
Sedative and Anesthetic Agents: What the Evidence Shows for ASD Populations
Dexmedetomidine — a selective alpha-2 adrenergic agonist — has emerged as one of the maximum extensively studied and applied sedative marketers in autistic pediatric populations, especially for methods which includes EEG recording, MRI, auditory brainstem reaction testing, and minor surgeries. Multiple guides together with research from Boston Children’s Hospital and a Frontiers in Psychiatry 2024 evaluation on intranasal dexmedetomidine for EEG in youngsters verify its medical utility, noting that intranasal dexmedetomidine has been proven to boom a hit sedation quotes in autistic youngsters for outpatient methods. Its mechanism — operating via alpha-2 receptors to provide sedation without breathing depression — makes it especially suitable for autistic sufferers in which breathing tracking in confined surroundings provides a challenge.
Midazolam, a benzodiazepine typically used for preoperative Anxiolysis, is broadly defined with inside the ASD anesthesia literature as a well-known premedication. However, medical case reports, which include an in-depth perioperative control case from PMC (PMC4916822), spotlight the crucial significance of course flexibility — oral, intranasal, and intramuscular alternatives ought to all be to be had and individualized — in addition to the involvement of dad and mom or caregivers with inside the management system to lessen procedural anxiety.
Notably, benzodiazepines paintings often through improving GABA-A receptor activity, and given the well-documented GABAergic dysregulation in ASD, nurses and prescribers ought to reveal cautiously for paradoxical reactions, which include accelerated agitation, hyperactivity, and disinhibit ion, which can be suggested greater regularly in autistic sufferers than in neurotypical populations.
Ketamine — a dissociative anesthetic — merits unique nursing interest inside the ASD context. While its maintenance of breathing force and simplicity of management (oral, intramuscular, or intravenous routes are all to be had) make it appealing for uncooperative or notably nerve-racking autistic sufferers, the Autism Research Institute explicitly increases medical issues approximately its use. Ketamine basically alters sensory perception, generating a hallucinogenic country that can be mainly distressing for autistic people whose sensory processing is already atypically organized.
Additionally, emergence effects — which include open eyes, nystagmus, and accelerated salivation — might also additionally make contributions to post-procedural dysregulation in autistic sufferers. Nurses administering ketamine to autistic sufferers ought to be organized for long and probably hard emergence duration and make certain that calm, consistent, acquainted aid is in region during recovery.
Propofol, a short-performing intravenous induction and upkeep agent, includes its personal concerns for autistic populations. Concerns were raised concerning propofol`s capacity to exacerbate mitochondrial dysfunction — a comorbidity with documented improved incidence in ASD — mainly with long-length or high-dose exposure. Nurses’ ought to record and talk any recognized mitochondrial prognosis or metabolic vulnerabilities to the anesthesia group before procedure. Nitrous oxide calls for similarly cautious consideration; its depletion of the B12 and float structures and inactivation of methionine synthase are mainly vast for autistic sufferers, who have a well-documented better incidence of methylation pathway vulnerabilities.
The Autistic SPACE Framework: A Nurse’s Perioperative Tool
The maximum critical strengthen in autism-conscious perioperative nursing care in 2024 and 2025 is the formalization of the Autistic SPACE framework, posted in BJA Education (February 2024) and encouraged throughout anesthesia and perioperative nursing practice. SPACE is an acronym representing the 5 middle domain names of individualized take care of autistic sufferers in perioperative settings: Sensory needs, Predictability, Acceptance, Communication, and Empathy.
From a nursing perspective, making use of SPACE starts off evolved on the preoperative evaluation stage, preferably through an established phone or in-individual interview with the affected person and their help community about forty-eight hours earlier than the system.
This evaluation need to seize sensory sensitivities — consisting of responses to light, sound, touch, temperature, and smell — due to the fact medical institution and theatre environments automatically reveal sufferers to bloodless blood stress cuffs, sturdy chemical odors from surgical prep and diathermy, unusual textures of robes and tracking equipment, and excessive ambient noise which could precipitate autistic crush earlier than a needle is located or an agent administered.
The BJA Education 2024 framework notes that autistic humans are often extraordinarily touchy to odors, occasionally perceiving smells that others cannot, making the olfactory surroundings of a perioperative suite a giant without difficulty, modifiable stressor.
Predictability is addressed via pre-system familiarization visits, visible schedules of the surgical pathway, and instruction of an individualized behavioral coping plan (BCP). Research funded with the aid of using the Organization for Autism Research (OAR) in 2025 at Duke Children`s Hospital and Dayton Children’s Hospital is actively evaluating effects among standard-of-care perioperative control and individualized adaptive sensory surroundings plus BCP care, particularly measuring preoperative tension degrees and sedation medicinal drug necessities at induction.
Preliminary information from Dayton Children’s, wherein each autistic infant gets customized perioperative adaptive sensory surroundings and BCP, helps that individualized instruction reduces procedural tension, which in flip might also additionally lessen the full sedative dose required to acquire ok preoperative anxiolysis.
Communication diversifications require nurses to decide the affected person’s number one communique modality earlier than the system — verbal, augmentative and opportunity communique (AAC) devices, image exchange, or signing — and to make certain that each one perioperative body of workers are briefed accordingly. The BJA Education framework similarly notes that autistic humans are much more likely to keep away from the usage of the phone, making the usual preoperative telecellsmartphone name a giant healthcare get admission to barrier that nurses and establishments need to proactively modify.
Nursing Responsibilities During Emergence: The Most Challenging Phase
Emergence from anesthesia is always defined with inside the ASD perioperative literature because the maximum clinically difficult section for autistic patients. The abrupt transition from unconsciousness to attention in an unfamiliar, stimuli-wealthy environment — blended with pain, nausea, thirst, disorientation, and lack of routine — creates a convergence of triggers that may precipitate intense dysregulation, together with emergence agitation, self-injurious behavior, and in a few instances bodily combativeness closer to workforce.
The BJA Education 2024 framework offers precise nursing steerage for emergence management: intravenous get entry to need to be securely bandaged or splinted earlier than the affected person wakes, non-crucial tracking needs to be eliminated earlier than emergence, and the affected person needs to be transferred to the healing trolley whilst nonetheless asleep every time possible. Padded cot facets are encouraged because of the threat of abrupt waking with capacity thrashing.
An acquainted caregiver or figure needs to be gift inside the healing place earlier than the affected person arrives, and scientific workforce should be organized to reduce bodily contact and discretion whilst defensive each the affected person and group from injury. Adequate analgesia, antiemetics, and hydration are crucial, because the BJA Education authors specially be aware that those unmet physiological wishes often force misery with inside the postoperative length and considerably impair the autistic affected person`s capacity to speak their wishes to nursing workforce.
Key Nursing Responsibilities across the Perioperative Continuum
Nurses preserve a principal and irreplaceable position at each level of perioperative takes care of autistic patients. In the preoperative section, the nurse’s duties consist of undertaking an individualized evaluation the usage of a based tool, figuring out conversation style, sensory triggers, behavioral history, modern medicines and recognized drug reactions, and any applicable comorbidity together with epilepsy, mitochondrial disease, and gastrointestinal situations that could have an effect on drug metabolism. Nurses should additionally short the entire surgical and anesthesia group on key individualized resorts and function the affected person’s number one endorse at some stage in the perioperative pathway.
During induction, the nurse’s position consists of assisting the selected induction strategy, facilitating parental presence as appropriate, minimizing environmental sensory input, and tracking for paradoxical reactions to premedication. Intraoperatively, nurses should make certain the anesthesia group is aware of ASD-precise drug concerns mentioned with inside the affected person’s care plan. In the postoperative section, the nurse is the primary scientific expert to greet the rising affected person in healing, making calm, acquainted, low-stimulation nursing presence arguably the maximum effective unmarried intervention with inside the whole perioperative pathway for this population.
Conclusion
Brain hyperconnectivity in ASD is a well-installed neurobiological phenomenon with direct, clinically big implications for sedation and anesthesia care. Autistic sufferers aren’t without a doubt behaviorally tough sufferers requiring heavier sedation — they’re neurologically awesome people whose odd cortical connectivity, E/I imbalance, sensory processing differences, and metabolic vulnerabilities call for individualized, cautiously titrated pharmacological care and a dependent, sensory-conscious perioperative environment.
In 2025, the Autistic SPACE framework and the developing frame of proof from establishments like Duke and Dayton Children`s Hospitals are reshaping perioperative nursing exercise for this population. For nursing students, practicing nurses, CRNAs, and perioperative educators, gaining knowledge of the neuroscience of ASD hyperconnectivity and its sedation implications is now a defining competency of safe, compassionate, and proof-primarily based totally care.
FAQs
FAQ 1: Does mind hyperconnectivity in ASD continually suggest autistic sufferers want decrease sedative doses?
Not necessarily. The proof is nuanced: a few autistic sufferers require better doses for procedural immobility, at the same time as others can be extra touchy to sure dealers because of underlying metabolic vulnerabilities. The key precept is individualized evaluation and cautious dose titration in place of making use of any blanket better or decreasing dose assumption to all autistic sufferers.
FAQ 2: What sedative agent is maximum normally endorsed for autistic youngster’s present process procedures?
Dexmedetomidine — especially through the intranasal route — has the most powerful proof base for procedural sedation in autistic pediatric sufferers, because it presents sedation without respiration melancholy and has proven excessive fulfillment quotes in ASD populations for EEG, MRI, and auditory brainstem reaction procedures. Midazolam is likewise normally used for preoperative anxiolysis, however calls for vigilance for paradoxical disinhibiting reactions.
FAQ 3: What is the Autistic SPACE framework and why is it vital for nurses?
Published in BJA Education in 2024, the Autistic SPACE framework is a dependent method to perioperative takes care of autistic sufferers protecting 5 domains: Sensory needs, Predictability, Acceptance, Communication, and Empathy. It courses nurses in accomplishing autism-conscious preoperative assessments, editing the perioperative environment, and coordinating individualized care that reduces anxiety, minimizes sedation requirements, and improves affected person and own circle of relative’s outcomes.
FAQ 4: Why is emergence from anesthesia especially tough for autistic sufferers?
Emergence combines more than one simultaneous stressors — pain, nausea, sensory overload, disorientation, and lack of routine — that may crush an autistic affected person’s regulatory capacity. This regularly produces emergence agitation and behavioral dysregulation. Nurses can mitigate this with the aid of making sure parental presence is recovery, minimizing environmental stimulation, securing IV get right of entry to earlier than emergence, and making sure good enough analgesia and antiemetics are administered proactively.
Read More:
https://nurseseducator.com/didactic-and-dialectic-teaching-rationale-for-team-based-learning/
https://nurseseducator.com/high-fidelity-simulation-use-in-nursing-education/
First NCLEX Exam Center In Pakistan From Lahore (Mall of Lahore) to the Global Nursing
Categories of Journals: W, X, Y and Z Category Journal In Nursing Education
AI in Healthcare Content Creation: A Double-Edged Sword and Scary
Social Links:
https://www.facebook.com/nurseseducator/
https://www.instagram.com/nurseseducator/
https://www.pinterest.com/NursesEducator/
https://www.linkedin.com/company/nurseseducator/
https://www.linkedin.com/in/afzalaldin/
https://www.researchgate.net/profile/Afza-Lal-Din
https://scholar.google.com/citations?hl=en&user=F0XY9vQAAAAJ